Collagen & Silicone Dressings · Clinical Reference · Southwest Florida
How to choose between collagen and silicone dressings
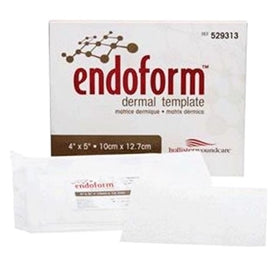
What does a collagen dressing do?
Collagen dressings provide the extracellular matrix scaffold that chronic stalled wounds lack. In a normal healing wound, the body produces collagen to support new tissue growth. In chronic wounds, elevated levels of matrix metalloproteinases (MMPs) break down collagen faster than the wound can produce it — stalling the healing process. Collagen dressings donate collagen directly to the wound bed, giving fibroblasts the structural framework they need to resume tissue regeneration. They are used when a wound has failed to show measurable progress over two or more weeks despite optimal standard dressing management.
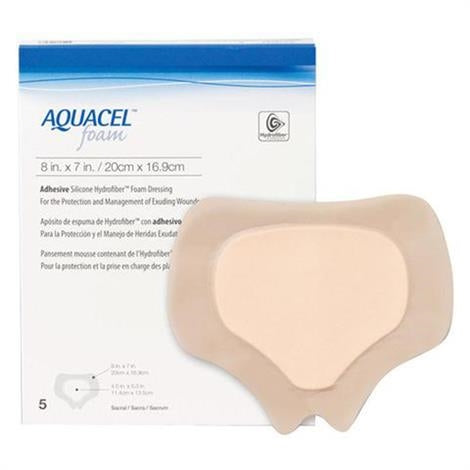
What is a silicone wound dressing used for?
Silicone dressings are designed for two main purposes: atraumatic dressing removal and protection of fragile or newly healed tissue. The silicone wound contact layer does not bond to the wound bed or periwound skin the way traditional adhesives do — it releases cleanly with minimal force, preventing the tearing and bleeding that standard dressings can cause on delicate tissue. They are the preferred choice for skin tears, partial-thickness burns, epithelializing wounds, pediatric patients, and any patient who reports significant pain at dressing changes.
When should I use a collagen dressing versus a silicone dressing?
The decision comes down to what problem you are solving. If the wound is chronic and stalled — not progressing despite two or more weeks of good wound care — collagen is the clinical tool to restart the healing process. If the wound is healing but the patient has fragile skin, is experiencing pain at changes, or has delicate new tissue that standard dressings are disrupting, silicone is the right choice. Many protocols use both: a collagen primary layer to stimulate healing, with a silicone secondary interface to protect the wound and allow atraumatic removal.
Can silicone dressings be reused?
Some silicone wound contact layers — particularly thin silicone interface sheets — are designed to be gently rinsed and reapplied for several dressing changes, making them highly cost-effective for wounds that need frequent changes. The secondary dressing covering the silicone layer is replaced at each change while the silicone interface stays in place or is reused. Always follow the specific manufacturer’s guidance on reuse, and discontinue if the silicone layer is damaged, soiled, or no longer releasing cleanly from the wound surface.
Are collagen dressings appropriate for infected wounds?
Collagen dressings are generally not used on clinically infected wounds. Active infection elevates MMP levels even further, which rapidly degrades the donated collagen before it can support healing — making the dressing ineffective until infection is controlled. For wounds showing signs of infection, address the bacterial burden first using antimicrobial dressings and clinician-guided systemic treatment where indicated. Once infection is resolved and the wound is clean but stalled, collagen dressings become an appropriate next step.
Commonly paired with collagen & silicone dressings
Collagen and silicone dressings are typically used with a secondary cover. Common combinations include:
Foam DressingsNon-Adherent DressingsAntimicrobial DressingsComposite DressingsMedical Tapes
For the full clinical picture on stalled wounds, collagen dressing protocols, and atraumatic dressing removal for fragile skin, see our Clinical Wound Care Guide →
Not sure whether collagen or silicone is right for your wound?
Our team is available by phone or in person at all five Southwest Florida locations — Venice · Sarasota · Port Charlotte · Fort Myers · Naples
Call 1-866-218-0902Find a Location